Celiac Disease
Pathology: Gluten triggers auto-antibody production and small intestinal atrophy.
Food-Symptom Interval: The pathological changes are delayed, so the connection between gluten and symptoms is not always obvious. However, once the patient is on a gluten-free diet, they may experience immediate digestive distress when consuming gluten.
Diagnosis: If the initial screening test (auto-antibody blood test) is positive, the diagnosis is confirmed with a small intestinal biopsy (looking for atrophy).
Treatment: The only remedy is a strict, lifelong gluten-free diet.
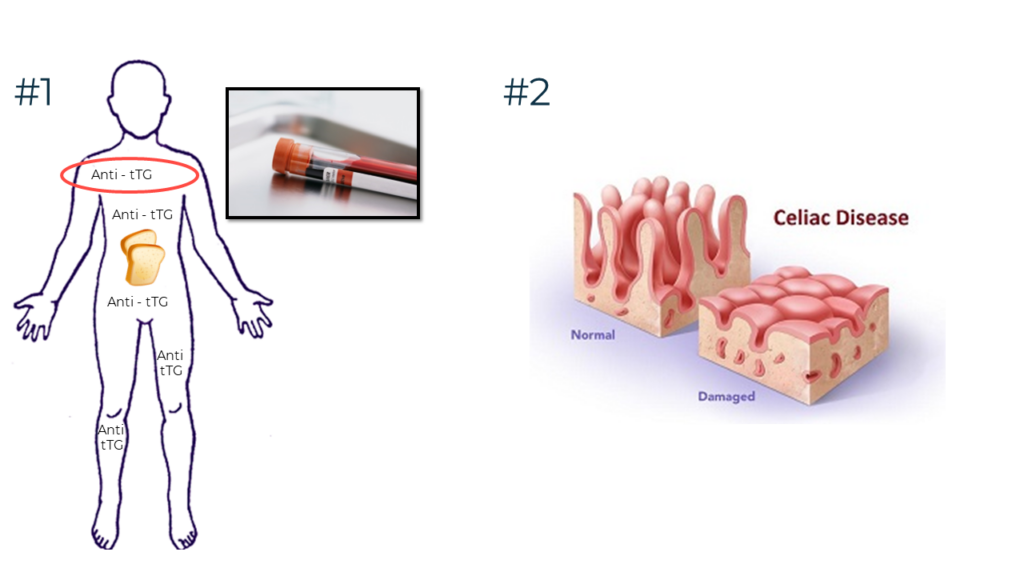
Celiac disease is an autoimmune condition. Gluten triggers the immune system to produce auto-antibodies directed against tissue transglutaminase (tTG), an enzyme in muscle tissue. The antibodies damage the entire body and the microvilli (small intestine) atrophies. This video gives a visual representation of these concepts.
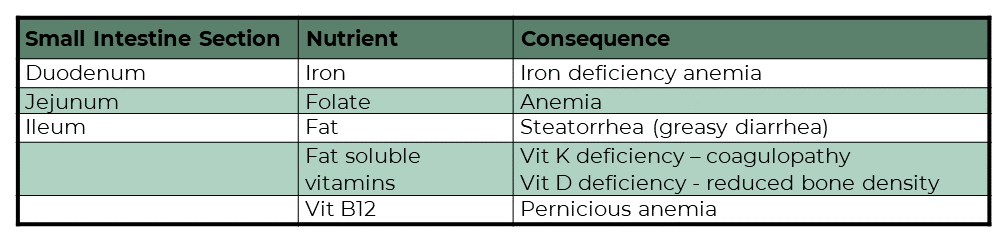
As discussed, celiac disease damages the entire body, so there is a long and diverse list of potential symptoms, including joint pain, dental enamel defects, iron deficiency anemia etc. Silent presentations (no signs) are also common.
Nutrient malabsorption also contributes to poor health and symptoms. The extent of malabsorption depends on the size and location of the atrophied patches.
Lactose intolerance is common in undiagnosed celiac disease and contributes to digestive symptoms. It usually resolves as the microvilli heal.
The diagnosis starts with a blood test to detect auto-antibodies. If the screening test is positive, the next step is a small intestinal biopsy to confirm villous atrophy. Celiac disease occursin about 1/100 of the general population, 1/20 In first-degree relatives, and 1/50 in second-degree relatives. First and second-degree relatives should be encouraged to request a screening test from their family doctor.
Diagnostic Difficulties
The diagnostic process can be complicated by:
- Patient eliminates gluten before testing: The autoantibody level decreases, and the intestine gradually heals on a gluten-free diet. After a few months, the test will be negative, even if the patient has celiac disease.
- Long wait for biopsy: A related problem is the client has a positive screening test but must wait several months for a biopsy. The client should stay on their regular diet. However, patients usually start a gluten-free diet, especially if they are not feeling well. Unfortunately, their intestine may heal, and the patient may not get a definitive diagnosis.
- IgA deficiency: The screening test measures IgA auto-antibodies. However, approximately 10% of celiac patients are IgA deficient, and the screen will be negative even if they have celiac disease. Most labs measure total IgA and use an alternative screening test if it is low. HCPs should check with their local lab to make sure this is done.
- Biopsy samples from healthy tissue: Celiac disease may be missed if the biopsy samples are taken from healthy tissue between the atrophied patches.
What to Do When Patients Eliminate Gluten Before Testing
A strict, life-long gluten-free diet requires a lot of effort—particularly avoiding foods with potential cross-contamination! When clients are unsure of their diagnosis, they may not be vigilant.
If the client has eliminated gluten before being tested for celiac disease, they can:
- Assume they have celiac disease and restrict accordingly: If other factors are suggestive, such as a history of typical symptoms (e.g., iron deficiency anemia) or strong family history, the client would be wise to live as if they have celiac disease.
- Go back to a gluten-containing diet: In my experience, very few clients agree to this if their symptoms have improved on a gluten-free diet. If they are willing, the next decision is how much gluten and how long they need to consume it for the auto-antibody level to rise and the microvilli to atrophy. There are no consensus or practice guidelines, and the best practice likely varies substantially between individuals.
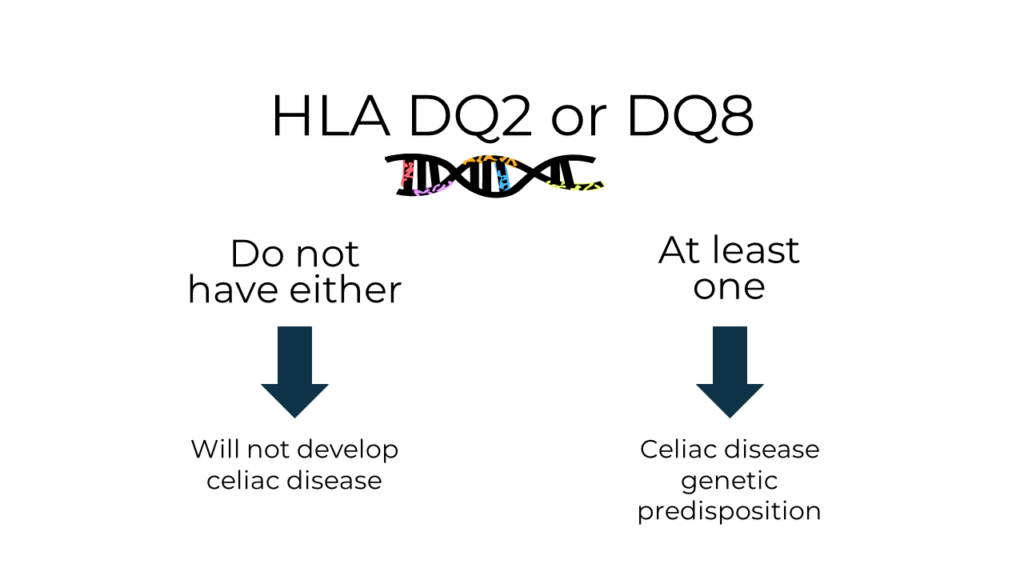
- HLA DQ2 & DQ8 genetic testing: If the client has neither gene, they do not have celiac disease (and never will). If they have at least one gene, they have a genetic predisposition. However, these genes are common and not specific to celiac disease.
Non-celiac gluten sensitivity is a subjective diagnosis given to clients who feel better on a gluten-free diet, but celiac disease has been ruled out. Some experts believe up to seven percent of the population is affected. However, no diagnostic markers exist to confirm who has and does not have this condition. There are many interesting theories about the potential pathology, but nothing conclusive.