Overview: The Vicious Cycle of Food Avoidance, Fear and Worsening Sensitivity
It’s easy to get caught up in trying to find the “perfect” diet to feel better. But this can often create confusion, frustration, and extra costs (like tests or supplements). It can also make food feel scary. Over time, this fear and restriction can turn into a vicious cycle – leading to a limited diet and more intense symptoms.
When the brain repeatedly associates certain foods with feeling unwell, the body may begin to react to those foods —even when the food itself is not causing physical damage or inflammation. This process is often described as conditioned food sensitivity.
Conditioned food sensitivity is not a medical diagnosis. Rather, it is a way of explaining how learned associations between foods and symptoms can develop through the mind–body connection. Viewing food sensitivity through this holistic lens can help broaden our understanding of how symptoms arise.
The ability for the brain to trigger reactions may sound questionable, but think of this lemon example:

Close your eyes and visualize cutting a lemon. Smell the citrus scent. Bring the lemon to your lips and squeeze a little juice on your tongue. Most people salivate when they do this visualization, demonstrating how the brain can create physical reactions based on associations.
It is important to note that biological causes of food reactions can also occur, including food allergies, celiac disease, lactose intolerance and other disorders.
The good news? You can change your brain’s food-illness associations and expand your diet!
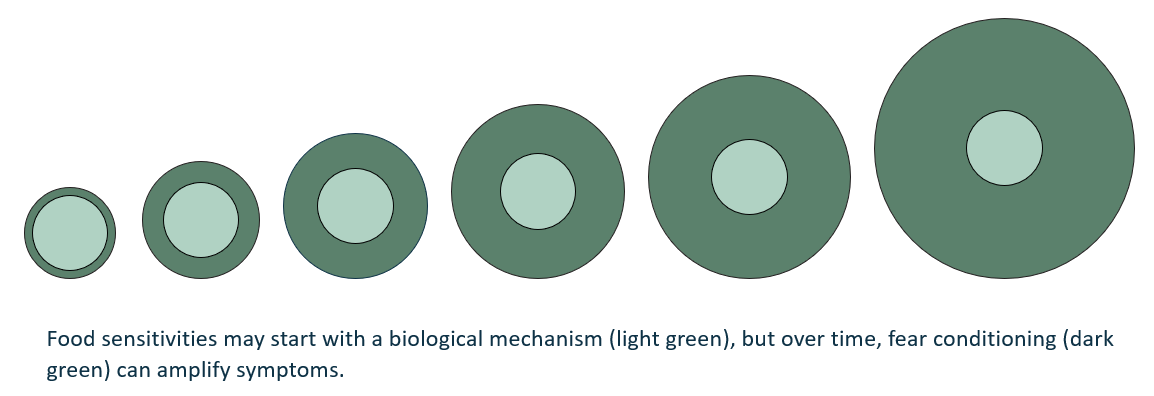
No, it is not in your head. Conditioned food sensitivity can produce real, physical symptoms—they are not imagined. That said, the brain plays an important role in this mind–body process. Some food sensitivities begin with a biological trigger, such as an illness, allergy, or disruption to digestion. Over time, stress, fear, and repeated negative experiences with food can increase the sensitivity of the nervous system, causing symptoms to feel more intense or occur more frequently.
This can create the impression that the body is becoming “sicker,” even when the underlying biological sensitivity remains relatively stable. In this way, the brain and nervous system can amplify symptoms through the mind–body connection, without those symptoms being “made up.”
Begin with small, compassionate shifts towards a better relationship with food. You don’t need to change everything at once. Here are a few simple ways to get started:
Avoiding foods can feel safe, especially if you’ve had difficult experiences. Over time, however, gradually expanding your diet can open the door to meaningful benefits:
There is no single “right” way to expand your diet – everyone’s journey is different. However, these strategies can help guide the process.
- Mikhael-Moussa H, Bertrand V, Lejeune E, et al. The Association of Avoidant/Restrictive Food Intake Disorder (ARFID) and Neurogastroenterology Disorders (Including Disorders of Gut-Brain Interaction [DGBI]): A Scoping Review. Neurogastroenterol Motil. Published online March 30, 2025. doi:10.1111/nmo.70039
- Weeks I, Abber SR, Thomas JJ, et al. The Intersection of Disorders of Gut-Brain Interaction With Avoidant/Restrictive Food Intake Disorder. J Clin Gastroenterol. 2023;57(7):651-662. Published 2023 Aug 1. doi:10.1097/MCG.0000000000001853.
- Hadamitzky M, Lückemann L, Pacheco-López G, Schedlowski M. Pavlovian Conditioning of Immunological and Neuroendocrine Functions. Physiol Rev. 2020;100(1):357-405. doi:10.1152/physrev.00033.2018.
- de Graaf MCG, Lawton CL, Croden F, et al. The effect of expectancy versus actual gluten intake on gastrointestinal and extra-intestinal symptoms in non-coeliac gluten sensitivity: a randomised, double-blind, placebo-controlled, international, multicentre study [published correction appears in Lancet Gastroenterol Hepatol. 2024 Mar;9(3):e8. doi: 10.1016/S2468-1253(24)00014-1]. Lancet Gastroenterol Hepatol. 2024;9(2):110-123. doi:10.1016/S2468-1253(23)00317-5.
- Wu J, Masuy I, Biesiekierski JR, Fitzke HE, Parikh C, Schofield L, Shaikh H, Bhagwanani A, Aziz Q, Taylor SA, Tack J, Van Oudenhove L. Gut-brain axis dysfunction underlies FODMAP-induced symptom generation in irritable bowel syndrome. Aliment Pharmacol Ther. 2022 Mar;55(6):670-682. doi: 10.1111/apt.16812. Epub 2022 Feb 15. PMID: 35166384.